Breathe Deeper: A Comprehensive Guide to Managing Asthma and COPD
Breathing is an act we perform without thinking, until it becomes difficult. For the millions of people living with chronic respiratory conditions, every gust of dust or a change in weather can feel like a threat. In Kenya, environmental factors like pollution, indoor wood-fire smoke, and seasonal allergens make the management of lung diseases particularly challenging.
The two most common obstructive airway diseases—**Asthma** and **Chronic Obstructive Pulmonary Disease (COPD)**—are often confused, but they require different approaches to long-term care. At LifeCare Hospitals, our Department of Respiratory Medicine is dedicated to moving beyond just "rescue" treatments toward building a life of unrestricted breathing. in this blog, we discussed the differences between these conditions and how our specialists can help you reclaim your lung capacity.
1. Understanding Asthma: The Sensitive Airway
Asthma is a chronic condition where the airways in the lungs become inflamed and narrowed in response to "triggers."
- What Happens: The muscles around the airways tighten, and the lining swells and produces extra mucus, making it hard to get air in and out.
- Common Triggers in Nairobi: Cold morning air, dust from unpaved roads, flowering plants (*pollen*), pet dander, and strong smells (like perfumes or cleaning supplies).
- Symptoms: Wheezing (a whistling sound), shortness of breath, a tight chest, and a persistent nighttime cough.
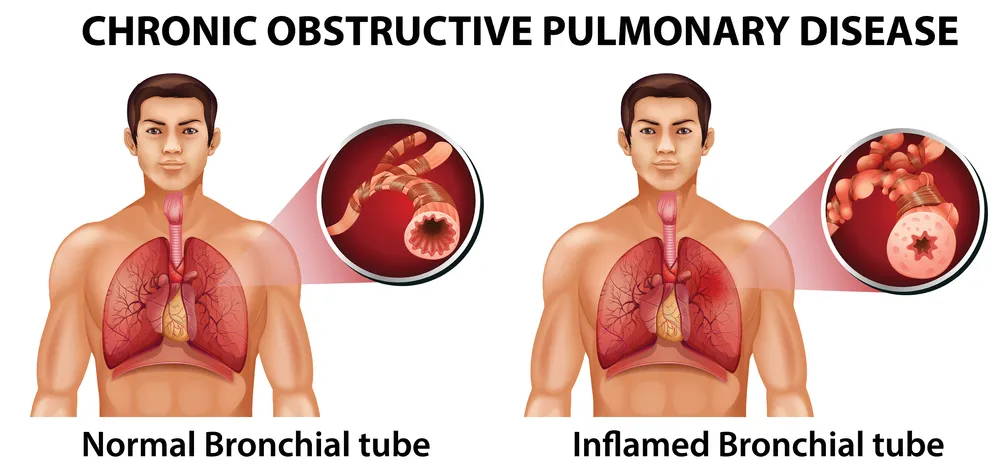
2. Understanding COPD: The Permanent Obstruction
COPD is an umbrella term that includes chronic bronchitis and emphysema.
- What Happens: The tiny air sacs in the lungs lose their elasticity, and the airways become permanently thickened and clogged. Unlike asthma, the blockage in COPD is not fully reversible.
- Main Causes in Kenya: Long-term smoking and exposure to "biomass" smoke—years of cooking with charcoal or wood in poorly ventilated kitchens.
- Symptoms: A chronic "smoker's cough" that produces mucus, blue-ish lips or fingernails (cyanosis), and debilitating shortness of breath even during mild exercise like walking.
3. How LifeCare Reclaims Your Breath: Diagnostics
You cannot treat what you haven't accurately measured. Our respiratory departments provide:
- Spirometry: A simple, painless test where you blow into a machine. It measures exactly how much air you can inhale and exhale, and how quickly you can do it. This is the gold standard for differentiating between asthma and COPD.
- Chest X-Ray / CT Scan: To look at the physical structure of the lungs and rule out other issues like pneumonia or lung cancer.
- Peak Flow Monitoring: We teach you how to use a small handheld device at home to monitor your lung function daily, so you know a "flare" is coming before you feel it.
4. Modern Management Strategies
Treatment is no longer just about carrying an inhaler.
- Controller vs. Rescue: We emphasize "Controllers" (daily medications that prevent inflammation) so that you rarely need your "Rescue" inhaler (the one for sudden attacks).
- Nebulization: For severe flare-ups, our departments provide specialized nebulization services that deliver medicine deep into the lungs using a fine mist.
- Inhaler Education: Many patients find their treatment "doesn't work" simply because of poor technique. Our nurses provide one-on-one training on the correct way to use MDI and DPI devices.
5. Pulmonary Rehabilitation: Strengthening the System
At LifeCare, we believe in a holistic approach.
For COPD patients especially, we offer **Pulmonary Rehabilitation**.
This is a program of supervised exercise and breathing techniques
designed to strengthen the muscles used for breathing. It doesn't "fix"
the lungs, but it makes your body more efficient, so you can do more
with the lung capacity you have.
6. Precision Respiratory Medicine at LifeCare Hospitals
Why choose LifeCare for your lung health?
- Consultant Pulmonologists: Our teams are led by specialists with years of experience in managed complex airway diseases.
- Allergy Testing: We help you identify your specific asthma triggers so you can avoid them systematically.
- Smoking Cessation: We provide the medical and psychological support needed to help you quit smoking, which is the single most important treatment for COPD.
Conclusion: Don't Settle for Labored Breathing
Breathing should be easy. If you are avoiding stairs, waking up at night coughing, or carrying a blue inhaler everywhere "just in case," your condition is not fully controlled.
LifeCare Hospitals Kenya is your dedicated partner in **Respiratory Excellence**. We are committed to ensuring that every breath you take is as clear and deep as possible. From children with intermittent asthma to seniors managing advanced COPD, our doors are open and our lungs are ready to help yours. Your brilliance is powered by oxygen; let's maximize the supply. Visit our respiratory department today for a lung function test. We are here to help you breathe easy again.
Frequently Asked Questions (FAQs)
Is Asthma curable?
**No, but it is 100% controllable.** With the right preventer medication, most asthma patients can live lives with NO symptoms, NO nighttime wake-ups, and the ability to exercise normally. Many children "grow out" of asthma as their lungs mature, but for adults, it is a life-long management journey.
Can a "non-smoker" get COPD?
**Yes.** In Kenya, a significant number of COPD cases in rural areas are caused by years of indoor cooking with wood or charcoal. Secondhand smoke and industrial air pollution are also risk factors.
Is it safe to exercise with asthma?
**Yes!** In fact, exercise is good for your lungs. If your asthma is well-controlled, you should be able to do any sport. If you have "exercise-induced" asthma, using your inhaler 15 minutes before you start typically prevents any symptoms.
Are inhalers addictive?
**No.** This is a dangerous common myth. Inhalers are not addictive. If you find yourself needing your inhaler more often, it doesn't mean you are "addicted"—it means your underlying lung disease is getting worse or is not well-controlled, and you need to see your LifeCare doctor to adjust your plan.
